As Parkinson’s disease rates rise worldwide, researchers are asking whether targeted supplements can influence inflammation, oxidative stress, mitochondria, and the gut microbiome, but the current evidence remains promising, mixed, and far from definitive.

Review: Dietary supplements for Parkinson's disease: State of the science. Image Credit: peterschreiber.media / Shutterstock
In a recent review published in the Journal of Parkinson’s Disease, a group of authors evaluated the disease-modifying potential of dietary supplements in Parkinson’s disease through evidence from human clinical trials. The review focused on clinical outcomes and biomarker-based evidence as proxy measures of disease modification, rather than definitive proof that supplements slow disease progression.
Background
Parkinson’s disease is the fastest-growing neurological condition worldwide, with prevalence projected to double by 2050. Medicines like levodopa are effective for controlling symptoms, but cannot prevent the continued loss of dopamine-producing brain cells that contribute to the progression of Parkinson’s disease.
Studies are also investigating how nutrients may reduce inflammation, oxidative stress, mitochondrial dysfunction, and changes in the gut microbiome linked to neurodegeneration. Many individuals with Parkinson’s disease already use supplements regularly despite limited clinical evidence. Further research is needed to identify which supplements truly slow disease progression.
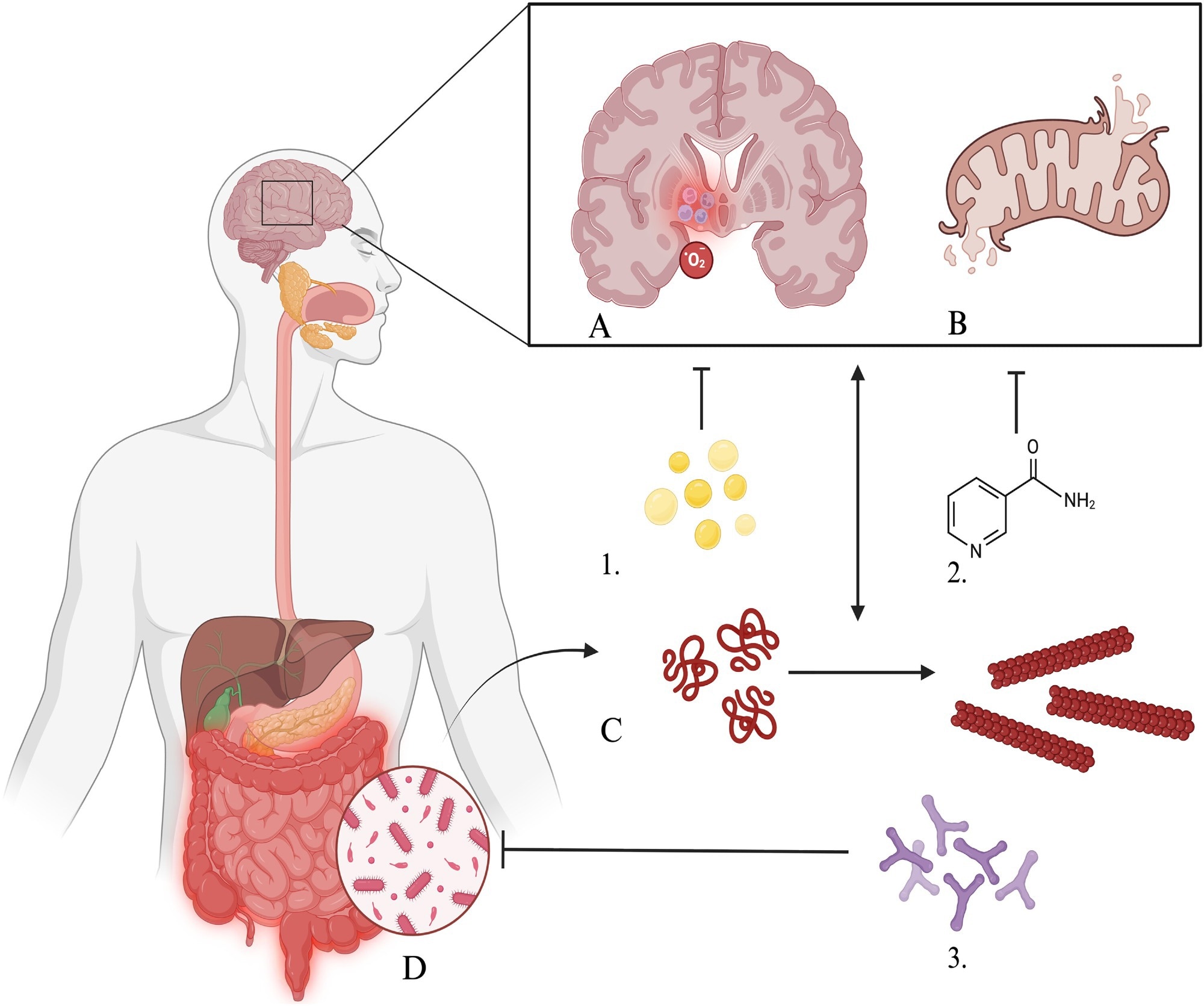
Primary mechanisms by which omega-3 fatty acids (n-3), nicotinamide riboside, and biotics influence key pathophysiological hallmarks of Parkinson’s disease. Inflammation, oxidative stress, and mitochondrial dysfunction are core, interconnected hallmarks that interact bidirectionally with α-synuclein aggregation. n-3 and NR may attenuate inflammation, oxidative stress, and mitochondrial dysfunction, whereas biotics modulate the gut microbiome, influencing α-synuclein aggregation and downstream pathways. Pathophysiological hallmarks: A, Neuroinflammation and oxidative stress; B, Mitochondrial dysfunction; C, α-synuclein aggregation; D, Gut dysbiosis. Interventions: 1, n-3; 2, NR; 3, Biotics.
Why dietary supplements matter?
Parkinson’s disease affects sleep, digestion, mood, thinking, and movement. This degenerative disorder is caused by the loss of dopamine-producing nerve cells and the buildup of toxic protein clumps, alpha-synuclein, in the brain. It is linked to factors such as chronic inflammation, oxidative stress, mitochondrial dysfunction, and changes in the gut microbiome. Dietary supplements have gained popularity as many have antioxidant or anti-inflammatory properties.
Omega-3 fatty acids show early promise
Omega-3 fatty acids are widely known for supporting heart health, but studies suggest they may also protect brain cells. Some clinical trials reported decreased markers of inflammation and improved antioxidant defenses as a result of omega-3 supplementation. In some studies, patients also showed improvements in Unified Parkinson's Disease Rating Scale scores.
However, studies showed inconsistent results, as omega-3 fatty acids also showed benefits in other trials when combined with vitamin E and/or other nutrients. Despite these study limitations, researchers argue that omega-3 fatty acids retain promise because they target multiple pathways involved in disease development, such as oxidative stress and inflammation.
B vitamins and nicotinamide riboside
B vitamins are essential for energy production and cellular metabolism. Nicotinamide riboside, a form of vitamin B3, is commonly used as it maintains mitochondrial function. Mitochondria, the powerhouses of the cell, are believed to play a role in the progression of Parkinson's disease.
Clinical studies indicate that high doses of nicotinamide riboside may improve MDS-UPDRS scores, particularly motor scores, but other trials have shown no clear clinical benefit, and disease modification remains unproven. Researchers noted that dosage differences may explain these conflicting findings. Studies using higher doses appeared more successful than those using lower doses.
Although the evidence remains limited, ongoing large-scale clinical trials may soon clarify whether nicotinamide riboside can truly slow disease progression. If successful, this supplement could inform future Parkinson’s disease management strategies.
Vitamins D and E produce mixed results
Vitamin D is known for its role in bone health, but it may also influence brain function and inflammation. One trial reported improvement in Hoehn and Yahr staging after vitamin D supplementation, but total UPDRS scores did not differ, and other studies have not shown consistent disease-modifying effects. The variability between the studies could have been due to different dosages used, body mass index (BMI), and different durations for which the studies were performed.
Although vitamin E can, in theory, reduce oxidative damage, studies have failed to demonstrate major improvements in disease progression when used alone. Later trials mainly tested vitamin E in combination with omega-3 fatty acids rather than as an independent treatment.
Creatine, coenzyme Q10, and curcumin
Several supplements once considered highly promising have delivered inconsistent or negative results in human studies. Creatine was hypothesized to support cellular energy and slow Parkinson’s disease progression, but large long-term trials failed to show disease-modifying benefit.
Coenzyme Q10 is another compound that supports mitochondrial function, and while small clinical studies have shown a reduction in Parkinson's progression, larger studies do not. The review also notes that coenzyme Q10 has been classified as non-efficacious for delaying Parkinson’s disease progression by major clinical guidance bodies.
Curcumin, a key component of the spice turmeric, is purported to have anti-inflammatory effects; however, at this time, there is only one small human pilot trial assessing curcumin for Parkinson’s disease progression, which found no significant improvement in total MDS-UPDRS or Hoehn and Yahr scores. Therefore, it cannot be assumed that curcumin is effective.
The gut microbiome and biotics
One of the most exciting areas of Parkinson’s disease research involves the gut microbiome. Many patients experience digestive problems years before motor symptoms appear, suggesting the gut may contribute to pathways involved in disease development. Research shows that people with Parkinson’s disease often have fewer beneficial bacteria that produce short-chain fatty acids.
Several studies show that probiotics reduced inflammation, improved antioxidant activity, and even lowered symptom severity scores. Evidence suggests that multi-strain probiotics may be generally more beneficial than single-strain probiotic formulations; possibly, because different bacteria perform complementary functions. Early studies suggest that some probiotic, prebiotic, and synbiotic interventions may influence gut barrier, inflammatory, and oxidative stress markers, as well as microbiome markers, but the evidence remains heterogeneous and limited, particularly for prebiotics.
Future directions in nutritional research
Researchers emphasized that no dietary supplement has yet been proven to stop Parkinson’s disease progression. However, some dietary supplements still have potential, including the combination of omega-3 fatty acids with vitamin E, nicotinamide riboside, and biotics.
Future research should use larger populations, longer follow-up periods, and more precise biomarkers to determine whether these interventions truly modify disease progression rather than merely temporarily improve symptoms. Furthermore, the authors suggest that research may need to test integrated approaches, potentially combining dietary supplements with broader lifestyle interventions such as diet and exercise.
Conclusions
Dietary supplements are increasingly being explored as supportive strategies that may help modify pathways linked to Parkinson’s disease progression.
Recent research suggests that biotics, nicotinamide riboside, and omega-3 fatty acids, combined with vitamin E, may have the potential to modulate inflammation, oxidative stress, mitochondrial dysfunction, and gut microbiome health, which are linked to neurodegenerative diseases. However, findings remain inconsistent, and many supplements, including creatine and coenzyme Q10, have failed to demonstrate reliable long-term benefits in larger clinical trials.
Researchers concluded that dietary supplements should not replace standard medical care but may complement future treatment strategies. Larger, longer, and methodologically stronger studies are required before definitive clinical recommendations can be made.
Download your PDF copy by clicking here.
Journal reference:
- Prasad, A., Shuler, M. S., Flanagan, R., Dayal, V., & Lithander, F. E. (2026). Dietary supplements for Parkinson's disease: State of the science. Journal of Parkinson’s Disease. DOI: 10.1177/1877718X261446386, https://journals.sagepub.com/doi/epub/10.1177/1877718X261446386