It has been nearly a year since the coronavirus disease 2019 (COVID-19) pandemic, caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) pathogen, was first detected in Wuhan, China. Since then, the virus has spread to over 191 countries and territories, infected over 64.36 million people, and claimed the lives of over 1.48 million.
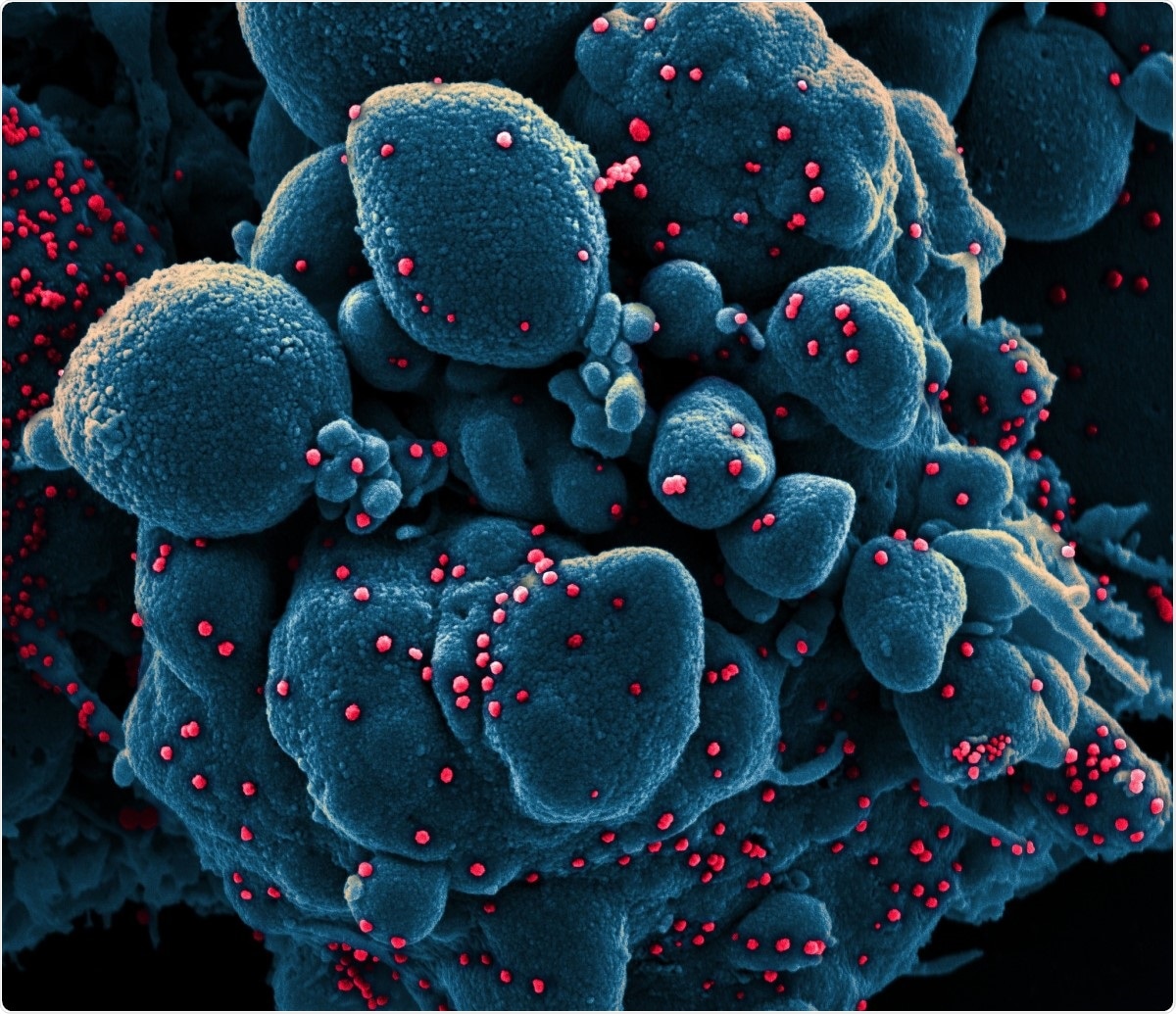
Novel coronavirus SARS-CoV-2. Colorized scanning electron micrograph of an apoptotic cell (blue) infected with SARS-COV-2 virus particles (red), isolated from a patient sample. Image captured at the NIAID Integrated Research Facility (IRF) in Fort Detrick, Maryland. Image Credit: NIAID / Flickr
The spread of COVID-19 has exacted an enormous toll on global public health and has had major ramifications for the world economy. As 2020 grinds to a close, the UK economy alone is projected to shrink by 11.3% due to the pandemic, and is forecast not to return to its pre-crisis size until late 2022. At present, the UK has reported 1.663 million cases and over 59,700 deaths. This has led many to describe the pandemic as the crisis of a generation. But is the end now in sight?
On December 2, following the Medicines and Healthcare products Regulatory Agency (MHRA) approval of the Pfizer vaccine, BNT162b1, the UK has announced its plan to commence targeted vaccinations for frontline healthcare workers, nursing home patients and those with underlying health conditions as early as December 7.
This targeted approach is aimed at protecting those most vulnerable to severe or critical COVID-19 (the elderly and those with potential comorbidities) as well as those most likely to become infected (healthcare workers) and transmit to others. When the capacity is available, the aim is to scale up the operation to the wider population in a phased priority approach depending on risk factors and other demographic considerations.
In being the first to roll out these vaccinations, the UK government believes it leads the charge in immunizing against SARS-CoV-2.
The Pfizer Vaccine
Early in November 2020, the large pharmaceutical company Pfizer, in collaboration with BioNTech, announced positive outcomes for their third and final phase of clinical trials, which involved human participants. The vaccine yielded an efficacy of 95%, significantly higher than the World Health Organization’s (WHO) recommended target of 70%.
MRHA, the UK's regulatory body, approves the Pfizer vaccine. Image Credit: Maria Kaminska / Shutterstock
While traditional vaccines typically inject an attenuated or inactivated version of the virus to elicit a robust immune response, the BNT162b1 vaccine – also known as ‘the Pfizer vaccine’ – is part of a new class of messenger ribonucleic acid (mRNA) vaccine that injects a part of SARS-CoV-2’s genetic material (mRNA) within a surrogate lipid envelope. The mRNA, which contains the message for building the spike protein essential for the SARS-CoV-2’s viral entry, then stimulates the host’s cells to produce the spike protein antigen. This then induces their immune system to produce neutralizing antibodies against it.
The development of RNA vaccines represents an enormous leap in nanotechnology; alongside the rival Moderna vaccine – also an mRNA-based model – the Pfizer vaccine has revolutionized pharmacological prophylactics in the space of less than a year. Not only might this change the course of the current pandemic, but it may also better equip us to tackle future outbreaks of similar viruses.
The regulatory body responsible for approving new drugs and medicines in the UK, the MRHA, had been reviewing the Pfizer vaccine since October 2020, when the results of its clinical trials were finalized and submitted for scientific scrutiny. The MRHA's decision was also made with advice from the Commission on Human Medicines (CHM), the government’s independent expert scientific advisory body. A dedicated team of MHRA scientists and clinicians carried out a rigorous, scientific and detailed review of all the available data.
This was done using a regulatory process known as a ‘rolling review’. A ‘rolling review’ can be used to complete the assessment of a promising medicine or vaccine during a public health emergency in the shortest time possible. This is done as the packages of data become available from ongoing studies on a staggered basis.
MHRA Chief Executive, Dr. June Raine said: “We have carried out a rigorous scientific assessment of all the available evidence of quality, safety, and effectiveness. The public’s safety has always been at the forefront of our minds – safety is our watchword.”
Challenges ahead
While this undoubtedly comes as a relief to many, the road to mass immunization is still a long way off. Not only does the vaccination process require two jabs, within 21 days of each other, but the vaccine needs to be stored at -70C before being administered, and the sheer volume of individuals needed to promote immunity will undoubtedly put a strain on the government’s ability to deliver in the timely manner required to begin offsetting the economic damage already done.
The government may also face resistance from members of the public skeptical about the efficacy and safety of the vaccine. They also fear the news may breed complacency at a time when non-pharmaceutical interventions remain crucial. Experts emphasize the need to remain vigilant and follow the rules to stop the virus from spreading – including social distancing, face mask-wearing and self-isolating – while the vaccination program gets underway. "We can't lower our guard yet," implores Prof Chris Whitty, the government's chief medical adviser.
Conclusion
"Today is a triumph for all those who believe in science," declares the UK’s Health Secretary Matt Hancock.
This is indeed a major development in the pharmacological fight against the COVID-19 pandemic; a moment many, including the government, have awaited with bated breath. Whether or not this marks the beginning of the end of the pandemic will depend on population compliance, a herculean logistical effort on the part of the government, and time needed to see how the vaccine's trial efficacy results hold up out in the population.
Sources:
Journal reference: