Multiple sclerosis (MS) is an autoimmune, acquired T cell-mediated neuro-inflammatory disorder that is marked by axonal degeneration and focal demyelination in the central nervous system (CNS).
Prevalence differs across different areas; in the United Kingdom prevalence is around 100 to 300 cases per 100,000 people. The disease typically occurs between the second and sixth decades of life with a female-to-male ratio of 2:1. In the majority of the people, there is an episodic (relapsing-remitting) course, where focal neurological symptoms and signs emerge over hours to days and progress over several weeks to months. Gradually, the frequency of relapses reduces and there is a propensity to develop progressive disabilities. In around 10% of patients, the disease is progressive, marked by the slow development of disability from onset. Diagnosis is performed on the basis of clinical evaluation as well as brain and spinal cord magnetic resonance imaging (MRI), and can be backed by cerebrospinal fluid analysis. There is a broad variety of immunomodulatory treatments that minimize relapse rates; however, it is still a challenge to develop effective therapies that can prevent long-term disability.
Neurobiology of Demyelination and Axon Degeneration
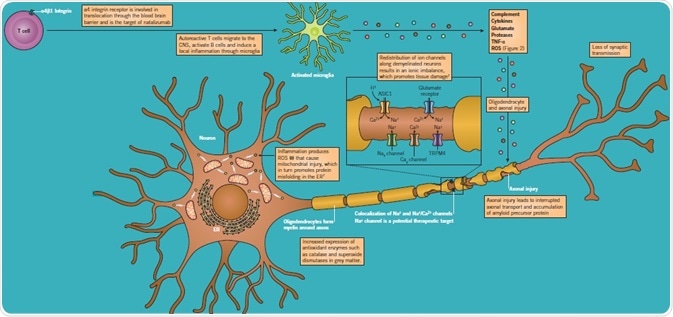
Figure 1: Mechanisms of demyelination and axon degeneration in MS. Image credit: Tocris Bioscience
The pathological characteristics of MS are demyelination, neuroinflammation, and axonal degeneration. Vital steps in these processes include activation of autoreactive T cells to myelin-related antigens, activation of CNS B cells, transition of immune cells through the blood-brain barrier, and microglial activation. The latter discharges reactive oxygen species (ROS; Figure 3), which are important mediators of cellular toxicity. In the inflammatory environment, oligodendrocytes are damaged leading to demyelination. Axonal injury takes place at an early stage and is progressive, disturbing axonal transport and the propagation of action potentials along the axon. Existing treatments target these processes, minimizing inflammatory activity with therapeutic effect.
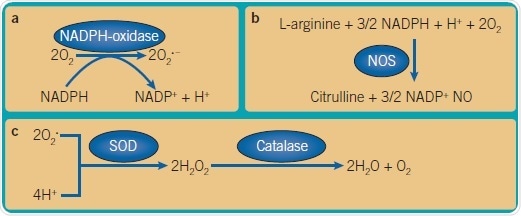
Figure 2. Important ROS reactions. (a) Generation of superoxide anion from molecular oxygen by NADPH (nicotinamide adenine dinucleotide phosphate)-oxidase as part of respiratory burst. (b) Generation of nitric oxide by action of nitric oxide synthases (NOS), in particular inducible NOS as part of the respiratory burst. (c) Detoxification of superoxide anion to oxygen and water through actions of superoxide dismutases (SODs) and peroxidases, for example, catalase. Image credit: Tocris Bioscience
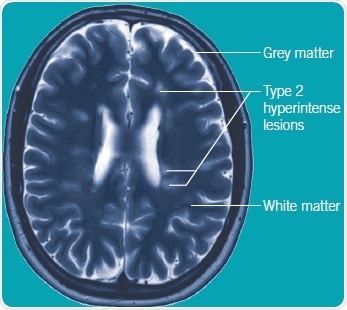
Figure 3. T2 weighted axial view of MRI brain scan from a patient with relapsing-remitting MS. Multiple white matter T2 hyperintense lesions are shown, in orientation and distribution typical for MS. Image credit: Tocris Bioscience
Genes and the Environment
Since 1865, when MS was first defined by Charcot, researchers and clinicians have considered the risk factors for developing MS. There is evidence of a polygenetic determinant of risk; specific human leukocyte antigen haplotypes bestow higher susceptibility. Furthermore, environmental factors like exposure to infectious agents may alter the risk of disease development.
Epidemiological investigations corroborate disparity in the occurrence of MS within and between countries, and a latitudinal gradient with a higher risk further from the equator. However, latitude alone fails to account for the intra-regional differences, which may be better defined by migration patterns and ethnicity-associated susceptibility. For example, there is a lower occurrence of MS in Americans with African ancestry than those with North European ancestry1.
Studies performed in twins2 substantiate a genetic determinant of risk that is polygenetic. In accordance with an autoimmune foundation to disease, HLA haplotypes, specifically DR2, have been recognized as susceptibility factors.
Epidemiological investigations reveal a link between MS risk and particular viral infections. Exposure to Epstein Barr virus over the course of an age-linked period of susceptibility is an environmental risk factor for MS. Furthermore, low vitamin D levels are associated with risk of relapse, and studies are evaluating whether vitamin D replacement impacts MS disease course.
Measuring Disease Activity and Disability
The concept of disease activity is vital to the understanding of an inflammatory basis for MS relapses. MR imaging with the potential to show subclinical CNS inflammation is a powerful tool in the measurement of disease activity (see Figure 3). In addition, loss of CNS volume (atrophy), estimated between interval scans, is also associated with the slow accrual of disability in progressive disease.
In order to evaluate potential treatment effects on progressive disease, it is vital to measure disability. Although initially established in 19613, the Expanded Disability Status Scale (EDSS) continues to be the de facto standard in clinical trials as a measure of disability. Similar to a primarily motor system-dependent scale that has non-linear ordinal characteristics, EDSS is an insensitive measure of variation in disability. The Multiple Sclerosis Functional Composite (MSFC) was designed to optimize this and it produces a parametric, continuous variable. MSFC enhances EDSS by formally evaluating cognition and being more sensitive to variation. Other prospective substitutes for disability, like optic coherence tomography, are being studied.
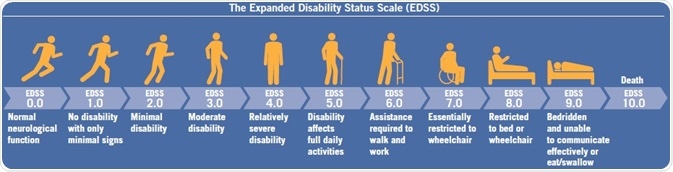
Figure 4: The Expanded Disability Status Scale (EDSS) for measuring progessive disability. Image credit: Tocris Bioscience
Drug Targets
Several licensed drug treatments are available for relapsing-remitting MS. These treatments minimize the burden of relapse. The first among these is Interferon β-1b (approved in 1993), which has moderate efficacy. Therapeutics that are more effective and often with a more substantial adverse event profile have been formulated—specifically, monoclonal antibodies. Oral agents with good tolerability and moderate efficacy, like teriflunomide and dimethyl fumarate, have further widened the available treatments. Although there has been progress, no significant randomized control trial evidence is available to indicate that any of these treatments have a considerable effect on long-term disability.
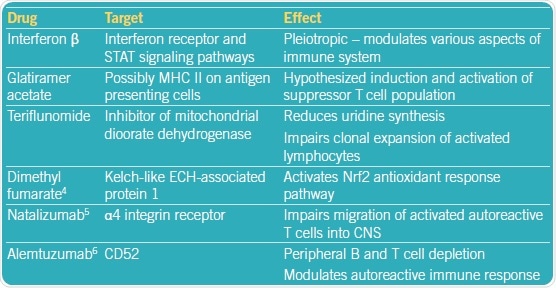
Figure 5: Experimental treatments for MS. Image credit: Tocris Bioscience
References
- Davenport (1921) Science 54 391
- Ebers (1982) The Lancet 2 1278
- Kurtzke (1961) Neurology 11 390
- Gold et al. (2012) NEJM 367 1098
- Polman et al. (2006) NEJM 356 899
- Cohen et al. (2012) Lancet 380 1819
- Dendrou et al. (2015) Nature 15 545
About Tocris Bioscience
Tocris Bioscience is your trusted supplier of high-performance life science reagents, including receptor agonists & antagonists, enzyme inhibitors, ion channel modulators, fluorescent probes & dyes, and compound libraries. Our catalog consists of over 4,500 research tools, covering over 400 protein targets enabling you to investigate and modulate the activity of numerous signaling pathways and physiological processes.
We have been working with scientists for over 30 years to provide the life science community with research standards, as well as novel and innovative research tools. We understand the need for researchers to trust their research reagents, which is why we are committed to supplying our customers with the highest quality products available, so you can publish with confidence.
Tocris is part of the protein sciences division of Bio-Techne, which also includes the best in class brands R&D Systems, Novus Biologicals, ProteinSimple, and Advanced Cell Diagnostics. Bio-Techne has united these brands to provide researchers with a full portfolio of research reagents, assays, and protein platforms. For more information on Bio-Techne and its brands, please visit bio-techne.com.
Sponsored Content Policy: News-Medical.net publishes articles and related content that may be derived from sources where we have existing commercial relationships, provided such content adds value to the core editorial ethos of News-Medical.Net which is to educate and inform site visitors interested in medical research, science, medical devices, and treatments.